-
 Epilepsy Program
Epilepsy Program
Ifakara, Wangin’gombe, Mbeya
Daima Mbele! – Always forward!
Epilepsy Program
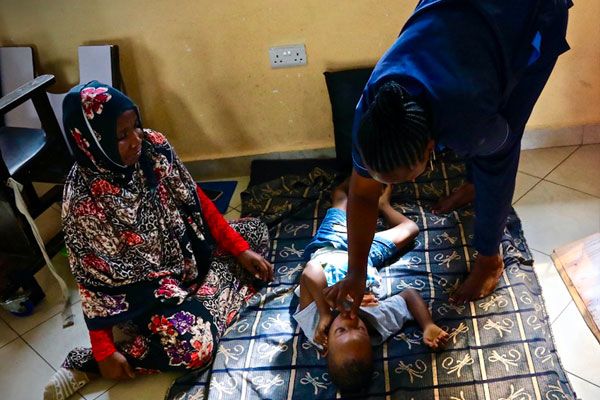
More than 50 million people worldwide live with epilepsy, of whom nearly 80 percent live in developing countries. 70 percent of people with epilepsy can lead seizure-free lives if properly diagnosed and treated, but in Tanzania, these people do not receive adequate treatment because there is a lack of specialized medical training in pediatric neurology. And, false myths and old superstitions about epilepsy also account for their social exclusion and discrimination.
In Inuka, SIMAMA, and A.Verna Kila Siku Rehabilitation Centers, about 55 percent of patients have epilepsy-related disorders: children with cerebral palsy go through this condition. Moreover, in addition to the problem of epilepsy for these children, there is the problem of malnutrition: in fact, individuals with neuromotor disabilities have a greater vulnerability to malnutrition for pathophysiological reasons (hormonal dysregulation, muscle spasticity, swallowing difficulties, etc.). The poverty of families and their lack of knowledge about appropriate nutrition certainly aggravate the clinical condition of children with epilepsy.

Clinic
Plans to start three outpatient clinics for the treatment of epilepsy at:
- the St. Francis Referral Hospital, in Ifakara in the Morogoro region
- the Inuka Rehabilitation Hospital, at Wangin’gombe in the Njombe region
- the Iyunga RC Health Center, at Mbeya in the Mbeya region of the same name.
Outpatient clinics will be equipped with diagnostic equipment such as electroencephalographs and medical drugs to treat the condition.
The start-up of the outpatient clinics will also be achieved through on-the-job training carried out by an Italian medical officer: training will be done to health personnel and caregivers directly involved in the care and treatment of children with epilepsy.

Training
Sponsored and managed by Saint Francis University College of Health and Allied Sciences at IFAKARA, a partner of Solidarity Communities in the World.
It aims to create a network of health professionals with specific knowledge of the mental health Gap Action Program (mhGAP) to share knowledge on diagnosis, treatment, and follow-up of epilepsy in resource-limited settings.
The training is conducted according to a cascade model: a Level 1 training targeting 40 health workers from 20 regions in Tanzania who will acquire the tools to repurpose in turn and in their home territories a Level 2 training with training stages targeting about 500 local health workers.
